Understanding Corns and Calluses
Corns and Calluses are both hardened layers of thickened skin that develop because of friction. Both ailments are typically found on the feet and may be unsightly. Although they have similarities, corns and calluses are different from each other.
Some causes of corns and calluses may be wearing ill-fitting shoes and not wearing socks. If you wear tight shoes, your feet will constantly be forced to rub against the shoes, causing friction. If you fail to wear socks, you are also causing your feet to endure excess friction.
There are some signs that may help you determine whether you have one of these two conditions. The first symptom is a thick, rough area of skin. Another common symptom is a hardened, raised bump on the foot. You may also experience tenderness or pain under the skin in addition to flaky, dry, or waxy skin.
There are also risk factors that may make someone more prone to developing corns and calluses. If you are already dealing with bunions or hammertoe, you may be more vulnerable to having corns and calluses as well. Other risk factors are foot deformities such as bone spurs, which can cause constant rubbing inside the shoe.
Corns tend to be smaller than calluses and they usually have a hard center surrounded by inflamed skin. They also tend to develop on the parts of the body that don’t bear as much weight such as the tops and sides of toes. Corns may also be painful for those who have them. On the other hand, calluses are rarely painful. These tend to develop on the bottom of the feet and may vary in size and shape.
Fortunately, most people only need treatment for corns and calluses if they are experiencing discomfort. At home treatments for corns and calluses should be avoided, because they will likely lead to infection. If you have either of these ailments it is advised that you consult with your podiatrist to determine the best treatment option for you.
What is a Corn?
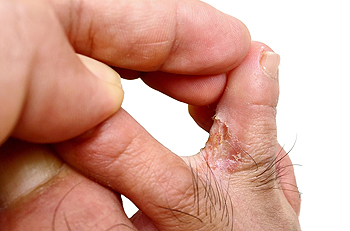 A corn can form on different parts of the foot as a result of excess friction. It is defined as a hard, thickened area, and will typically cause severe pain and discomfort. If the shoes that are worn do not fit properly, a corn may form on the inside of the pinky toe. Relief may be found if a pad is worn over the affected area. Additionally, it may help to soak the affected foot in warm water, as this may aid in softening the corn. Afterward, a pumice stone can be used in gently filing the corn to remove any dead skin. When toenails are properly trimmed, pressure may be avoided from the nail touching the skin, and this may help to prevent corns from developing. If you are afflicted with corns, it is suggested that you seek the counsel of a podiatrist who can assist you in choosing the proper treatment.
A corn can form on different parts of the foot as a result of excess friction. It is defined as a hard, thickened area, and will typically cause severe pain and discomfort. If the shoes that are worn do not fit properly, a corn may form on the inside of the pinky toe. Relief may be found if a pad is worn over the affected area. Additionally, it may help to soak the affected foot in warm water, as this may aid in softening the corn. Afterward, a pumice stone can be used in gently filing the corn to remove any dead skin. When toenails are properly trimmed, pressure may be avoided from the nail touching the skin, and this may help to prevent corns from developing. If you are afflicted with corns, it is suggested that you seek the counsel of a podiatrist who can assist you in choosing the proper treatment.
If you have any concerns regarding your feet and ankles, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Dr. Shlonsky to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What is Tarsal Tunnel Syndrome?
 Tarsal tunnel syndrome occurs in the foot and ankle. It is similar to carpal tunnel syndrome, which occurs in the wrist. Both disorders arise from the compression of a nerve in a confined space. Tarsal tunnel syndrome is a constriction, or squeezing, on the posterior tibial nerve that produces symptoms anywhere on the path of the nerve running from the inside of the ankle into the foot. The posterior tibial nerve is the focus of tarsal tunnel syndrome. This nerve runs down the back of the calf and into the sole of the foot. When tissues around the tarsal tunnel become inflamed, they can swell and press on the nerve, causing severe pain. If you have pain in your foot or ankle and want to identify the source, it is suggested to consult with your local podiatrist. Your podiatrist may prescribe corticosteroid injections, orthoses, and in some cases, surgery to treat this ailment.
Tarsal tunnel syndrome occurs in the foot and ankle. It is similar to carpal tunnel syndrome, which occurs in the wrist. Both disorders arise from the compression of a nerve in a confined space. Tarsal tunnel syndrome is a constriction, or squeezing, on the posterior tibial nerve that produces symptoms anywhere on the path of the nerve running from the inside of the ankle into the foot. The posterior tibial nerve is the focus of tarsal tunnel syndrome. This nerve runs down the back of the calf and into the sole of the foot. When tissues around the tarsal tunnel become inflamed, they can swell and press on the nerve, causing severe pain. If you have pain in your foot or ankle and want to identify the source, it is suggested to consult with your local podiatrist. Your podiatrist may prescribe corticosteroid injections, orthoses, and in some cases, surgery to treat this ailment.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Treating Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which the tibial nerve, located in the tarsal tunnel in the foot, is compressed. The tibial nerve can become compressed from injury, such as an ankle sprain, flat feet, and lesions. Arthritis, diabetes, and varicose veins can also cause swelling and thus result in nerve compression.
Symptoms of tarsal tunnel syndrome include several different sensations in the sole of the foot, inside the ankle, and around the tibial nerve. These sensations include shooting pains, numbness or reduced sensation, pins and needles, burning, and tingling. Symptoms tend to worsen with greater activity to the area. In rare and severe occasions, this can change the muscles in the foot.
If you suspect you have tarsal tunnel syndrome, you should consult with your podiatrist. He or she will examine your medical history to see if you have a history of diabetes, arthritis, or flat feet. They will also check to see if you have suffered an injury to the area recently. An electrical test will be conducted to check if the nerve has been damaged. A simpler Tinel’s Test might also be used. This includes simply tapping the nerve to create a sensation. An MRI scan of the area may also be used.
Treatments vary greatly for tarsal tunnel syndrome. Treatments include both nonsurgical and surgical options depending upon the severity of the condition. Nonsurgical options include anti-inflammatory medication and steroid injections to the area. Orthotics, such as a splint or brace that immobilizes the foot, is another noninvasive option. For those with flat feet, custom shoes can be made to offer better foot support. Surgical options include a tunnel tarsal release, in which an incision is made behind the ankle down to the arch of the foot. This releases the ligament and relieves pressure off the nerve. Some doctors use a more minimally invasive surgery, where smaller incisions are made in the ankle and the ligament is stretched out.
If you are suffering from painful sensations in your foot, see a podiatrist who can determine if you are experiencing tarsal tunnel syndrome. Tarsal tunnel syndrome that is left unchecked can cause permanent nerve damage to the foot.
Helpful Tips On Elderly Foot Care
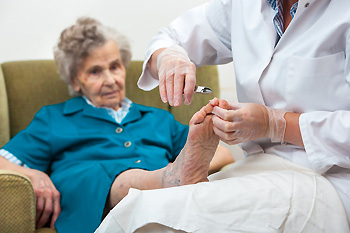 Research has shown the importance for elderly people to properly take care of their feet. It may be difficult for seniors to bend down to trim their toenails, and they may benefit from having a caregiver or a relative help them accomplish this. If the patient is diabetic, any cuts, scrapes, or wounds on the feet need to be treated as quickly as possible. This can be helpful in preventing any infections from developing. Additionally, wearing socks that fit properly may be helpful controlling existing circulation conditions. The feet may change size as the aging process occurs, and it is suggested that the feet get measured regularly. This will help in determining the correct shoe size that will be comfortable to wear. Elderly patients may find it feels good to frequently stretch their feet, and this may benefit the overall health of the feet. If you would like additional information about how to help geriatric patients properly care for their feet, it is suggested that you consult with a podiatrist.
Research has shown the importance for elderly people to properly take care of their feet. It may be difficult for seniors to bend down to trim their toenails, and they may benefit from having a caregiver or a relative help them accomplish this. If the patient is diabetic, any cuts, scrapes, or wounds on the feet need to be treated as quickly as possible. This can be helpful in preventing any infections from developing. Additionally, wearing socks that fit properly may be helpful controlling existing circulation conditions. The feet may change size as the aging process occurs, and it is suggested that the feet get measured regularly. This will help in determining the correct shoe size that will be comfortable to wear. Elderly patients may find it feels good to frequently stretch their feet, and this may benefit the overall health of the feet. If you would like additional information about how to help geriatric patients properly care for their feet, it is suggested that you consult with a podiatrist.
If you need your feet checked, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky will attend to all of your foot and ankle needs and provide you with quality treatment.
Geriatrics and Podiatry
When people age, some common issues that may occur are bone density loss, dry skin, poor circulation, and rough brittle nails. These issues may also affect your foot health if the necessary steps are not taken to alleviate the problems.
It is important to take care of your feet because feet that are injured or diseased can affect your overall health. Having painful feet hinders your ability to do daily activities or may decrease your willingness to do the things that you need to do.
Visiting Your Geriatrician
As we age, health problems become more likely, so it is essential to visit your doctor for check-ups to ensure that you are doing the best you can to take care of your health. It is recommended to check your feet frequently for any possible cuts, bruises, swelling, corns or any other irregularities.
Taking Care of Elderly Feet
Cracked or dry feet can be treated by applying moisturizer often. It is also important not to wear old socks because the older the sock is, the higher the possibility there will be that there is bacteria there. Wear fresh socks and make sure they fit properly.
Proper foot health means that you can have a more active lifestyle and you will not be bogged down by pain. Foot health also leads to good circulation, which is paramount for overall health.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Geriatrics and Podiatry
Bone density loss, dry skin, poor circulation, and rough and brittle nails are some of the common problems that can occur as people age. The effect that these problems has on foot health should be of particular concern in comprehensive geriatric care.
Feet that are diseased or injured have a negative effect on overall health and safety. Painful feet limit a person’s willingness and ability to stay active. Poor foot health can also cause gait change, which can lead to falls and accidents. Even though recovery time from health problems naturally slows as we age, many foot problems can be avoided altogether with regular prophylactic care.
Feet should be thoroughly washed in warm water daily. Care must be taken to dry the feet well, making sure to dry between and under the toes. Any left-over moisture can cause problems like foot fungus. After cleaning feet carefully check for problems such as cracked skin, bruises, swelling, cuts, corns, or other irregularities.
Examine toenails for ingrown, jagged, or split nails. Long toenails should be cut straight across. Never cut toenails at an angle or down the side as this may lead to ingrown nails.
Cracked and dry feet should be treated once or twice a day with a non-greasy moisturizer. Rub the moisturizer into the skin and allow it to dry before putting on socks and shoes. Sweaty feet can be dusted with a small amount of talcum powder. Avoid putting talcum directly into shoes as this may make feet slip within the shoe and cause a serious fall.
Wear clean dry socks each day. Not only do clean socks feel better on the feet, but socks worn for longer periods may harbor disease and odor-causing bacteria. Socks should not be tight around the top as they can leave marks on the leg. Socks that are too small can bring about bruising caused by pressure against the toes.
Wear comfortable and well-fitting shoes. If possible, consult a professional footwear specialist when purchasing shoes. Do not walk around barefoot as this exposes the feet to possible injury and bacteria.
Good foot health allows a more active lifestyle, which improves blood flow. Good circulation aids in recovery from injury or illness. It is also important for maintaining overall health.
Serious health problems can manifest themselves as symptoms in the feet. The elderly should seek professional help from a podiatrist if experiencing foot problems like tingling, numbness, pain, infection, or a sore that does not heal. Taking care of these problems right away can prevent the development of severe cases.
How Can Poor Circulation Be Improved?
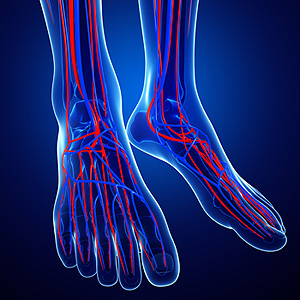 The symptoms that often accompany poor circulation can include a tingling and numbing sensation in the hands and feet, swollen toes, and toenails may be brittle and discolored. Some patients experience dry skin, dizzy spells and headaches, and these may be indicative of this condition. Raynaud’s disease is a type of poor circulation, and this may cause the fingers and toes to turn white, and may feel cold for the majority of the day. It is helpful to know that symptoms of circulation conditions may be diminished by performing a gentle exercise routine as frequently as possible. This may help to improve blood flow in the body. Additionally, it may be beneficial to limit or stop smoking, which may stop the arteries from becoming narrow. If you would like to learn more about how poor circulation can affect the feet, please schedule an appointment with a podiatrist.
The symptoms that often accompany poor circulation can include a tingling and numbing sensation in the hands and feet, swollen toes, and toenails may be brittle and discolored. Some patients experience dry skin, dizzy spells and headaches, and these may be indicative of this condition. Raynaud’s disease is a type of poor circulation, and this may cause the fingers and toes to turn white, and may feel cold for the majority of the day. It is helpful to know that symptoms of circulation conditions may be diminished by performing a gentle exercise routine as frequently as possible. This may help to improve blood flow in the body. Additionally, it may be beneficial to limit or stop smoking, which may stop the arteries from becoming narrow. If you would like to learn more about how poor circulation can affect the feet, please schedule an appointment with a podiatrist.
Poor circulation is a serious condition and needs immediate medical attention. If you have any concerns with poor circulation in your feet contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky will treat your foot and ankle needs.
Poor Circulation in the Feet
Poor blood circulation in the feet and legs is can be caused by peripheral artery disease (PAD), which is the result of a buildup of plaque in the arteries.
Plaque buildup or atherosclerosis results from excess calcium and cholesterol in the bloodstream. This can restrict the amount of blood which can flow through the arteries. Poor blood circulation in the feet and legs are sometimes caused by inflammation in the blood vessels, known as vasculitis.
Causes
Lack of oxygen and oxygen from poor blood circulation restricts muscle growth and development. It can also cause:
- Muscle pain, stiffness, or weakness
- Numbness or cramping in the legs
- Skin discoloration
- Slower nail & hair growth
- Erectile dysfunction
Those who have diabetes or smoke are at greatest risk for poor circulation, as are those who are over 50. If you have poor circulation in the feet and legs it may be caused by PAD and is important to make changes to your lifestyle in order to reduce risk of getting a heart attack or stroke. Exercise and maintaining a healthy lifestyle will dramatically improve conditions.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes Symptoms and Treatment for Poor Circulation in the Feet
The purpose of the body’s circulation system is to transport blood, oxygen, and nutrients throughout the body. A reduction of blood to a specific part of the body may cause one to experience symptoms of poor circulation. The most common causes of poor circulation in the feet are obesity, diabetes, and heart conditions such as peripheral artery disease (PAD). Common symptoms of poor circulation include tingling, numbness, throbbing, pain and muscle cramps.
Peripheral artery disease is a common cause of poor circulation in the legs. Symptoms of PAD are cramping, pain or tiredness in the leg or hip muscles while walking or climbing stairs. This pain tends to go away with rest and starts back up when you begin to walk. It is a condition that causes the blood vessels and arteries to become narrow. Although PAD is more common in adults over the age of 50, it may also occur in younger people. A similar condition called atherosclerosis causes arteries to stiffen up due to a buildup of plaque in the arteries and blood vessels.
Blood clots are also a common cause of poor circulation in the feet. Clots may obstruct blood vessels and if they occur in the legs, they may eventually lead to pain and discoloration. This occurrence is commonly known as deep vein thrombosis (DVT) and it may travel to the lungs. Varicose veins are another condition that may lead to poor circulation, and it is caused by incompetence of the valves in the veins. Women who are overweight are prone to developing this condition. Lastly, diabetes, which is correlated with poor blood sugar metabolism may lead to chronic poor circulation. Those with diabetes often suffer from cramping in the legs, calves, thighs and buttocks.
If you are looking for ways to avoid poor circulation there are some tips you can follow. One tip is to avoid sitting for too long. If you plan to sit down for a long period of time, you should try standing up occasionally, to improve your circulation. Another great way to avoid poor circulation is to exercise. Exercise is an excellent way to pump the heart and increase blood flow. Those who suffer from poor circulation should also avoid smoking, reduce their salt intake, and try to lose weight.
If you are experiencing symptoms from poor circulation in your feet, you should consult with your podiatrist to determine the best method for treatment for you. He or she may prescribe medication in addition to recommending specific lifestyle changes to improve your circulation.
Washington Baseman Deals with Plantar Fasciitis Recovery
 First baseman Ryan Zimmerman of the Washington Nationals has suffered a “brutal” season due to plantar fasciitis in his right foot. The condition made Zimmerman’s returns to the field slow. The nature of the athlete’s injury has also made it slow to heal; fully torn plantar fascia are faster to heal, but Zimmerman’s fascia was only partly torn. Before his return on September 1st, Zimmerman rehabilitated on the treadmill. Plantar fasciitis is a common sports injury that can be disruptive to everyday life. If you think you’ve sustained a plantar fasciitis injury, contact your podiatrist.
First baseman Ryan Zimmerman of the Washington Nationals has suffered a “brutal” season due to plantar fasciitis in his right foot. The condition made Zimmerman’s returns to the field slow. The nature of the athlete’s injury has also made it slow to heal; fully torn plantar fascia are faster to heal, but Zimmerman’s fascia was only partly torn. Before his return on September 1st, Zimmerman rehabilitated on the treadmill. Plantar fasciitis is a common sports injury that can be disruptive to everyday life. If you think you’ve sustained a plantar fasciitis injury, contact your podiatrist.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.








