
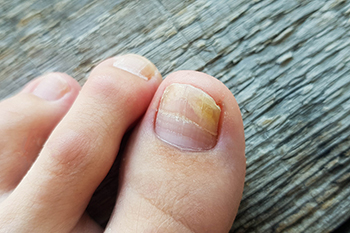
Experiencing toenail fungus, or onychomycosis, can be a persistent and bothersome condition. Toenail fungus causes nails to become yellow, opaque, and brittle, often leading to crumbling or breaking. The fungus thrives in warm, moist environments, making individuals with sweaty feet or those who wear heavy shoes more susceptible. Not only is it unpleasant, but toenail fungus is also highly contagious. It can spread easily in communal areas, such as swimming pools, locker rooms, and shared showers. Treatment usually involves oral antifungal medications that need to be taken for several weeks. Even as the medication starts working, it might take some time before new, healthy nail growth appears, and the discoloration and brittleness may persist until then. Preventive measures are essential to managing and avoiding the spread of the infection. Keeping feet dry, wearing moisture-wicking socks, trimming nails properly, and ensuring feet are fully dry before putting on socks and shoes can help. If you are experiencing symptoms of toenail fungus, it is suggested that you make an appointment with a podiatrist for an exam and treatment.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Symptoms
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
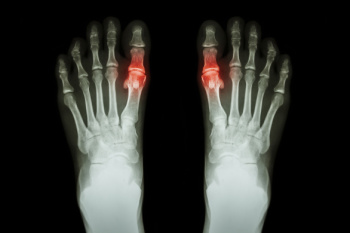 Gout is a type of arthritis caused by the accumulation of uric acid crystals in the joints, often affecting the feet, particularly the big toe. It leads to sudden, severe pain, in addition to redness and swelling. Gout predominantly affects middle-aged men and postmenopausal women, especially those with a diet high in purines, a substance found in red meat and alcohol. The condition is often diagnosed through blood tests measuring uric acid levels and joint fluid analysis to detect urate crystals. Treatment focuses on reducing pain and inflammation with nonsteroidal anti-inflammatory drugs, corticosteroids, or colchicine. Long-term management includes medications like allopurinol or febuxostat to lower uric acid levels. For foot-specific care, patients may elevate the affected foot and wear comfortable, supportive footwear to alleviate symptoms and prevent flare-ups. Preventing gout involves maintaining a healthy diet, staying hydrated, and avoiding foods high in purines. Regular exercise and weight management are also critical. If you have gout that is negatively impacting your feet, it is suggested that you consult a podiatrist for specialized care and tailored advice.
Gout is a type of arthritis caused by the accumulation of uric acid crystals in the joints, often affecting the feet, particularly the big toe. It leads to sudden, severe pain, in addition to redness and swelling. Gout predominantly affects middle-aged men and postmenopausal women, especially those with a diet high in purines, a substance found in red meat and alcohol. The condition is often diagnosed through blood tests measuring uric acid levels and joint fluid analysis to detect urate crystals. Treatment focuses on reducing pain and inflammation with nonsteroidal anti-inflammatory drugs, corticosteroids, or colchicine. Long-term management includes medications like allopurinol or febuxostat to lower uric acid levels. For foot-specific care, patients may elevate the affected foot and wear comfortable, supportive footwear to alleviate symptoms and prevent flare-ups. Preventing gout involves maintaining a healthy diet, staying hydrated, and avoiding foods high in purines. Regular exercise and weight management are also critical. If you have gout that is negatively impacting your feet, it is suggested that you consult a podiatrist for specialized care and tailored advice.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
Risk Factors
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Gout, typically found in diabetic patients, is an unusually painful form of arthritis caused by elevated levels of uric acid in the bloodstream. The condition typically strikes the big joint on the big toe. It has also been known to strike the knees, elbows, fingers, ankles and wrists—generally anywhere that has a functioning, moving joint.
The high level of uric acid in a person’s bloodstream creates the condition known as hyperuricema—the main cause of gout. Genetic predisposition occurs in nine out of ten sufferers. The children of parents who suffer gout will have a two in ten chance of developing the condition as well.
This form of arthritis, being particularly painful, is the leftover uric acid crystallizing in the blood stream. The crystallized uric acid then travels to the space between joints where they rub, causing friction when the patient moves. Symptoms include: pain, redness, swelling, and inflammation. Additional side effects may include fatigue and fever, although reports of these effects are very rare. Some patients have reported that pain may intensify when the temperature drops, such as when you sleep.
Most cases of gout are easily diagnosed by a podiatrist’s assessment of the various symptoms. Defined tests can also be performed. A blood test to detect elevated levels of uric acid is often used as well as an x-ray to diagnose visible and chronic gout.
Treatment for gout simply means eliminating symptoms. Non-steroid anti-inflammatory drugs or NSAIDs (Colchicine and other corticosteroid drugs, etc.) will quell the redness, the swelling, and the inflammation. However, managing your diet, lifestyle changes, and using preventative drugs are all helpful toward fully combating the most severe cases.
Those that lead an inactive lifestyle are at a higher risk for gout. Any amount of exercise decreases the probability of repeat encounters with the condition. Reducing your consumption of red meat, sea food, and fructose-sweetened drinks also reduces the likelihood of chronic gout as well.
Ingesting Vitamin C, coffee, and particular dairy products can help with maintaining a healthy lifestyle. There are new drugs out on the market that inhibit the body’s production of uric acid-producing enzymes. However, reducing or eliminating your overall levels of uric acid is the best remedy to ensuring you lead a gout-free life.
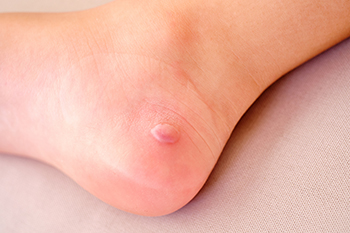 Friction blisters of the feet are painful lesions caused by repetitive rubbing against the skin. These blisters typically occur on areas of the feet that experience frequent pressure or friction, such as the heels or toes. They appear as fluid-filled sacs beneath the top layer of skin and may cause discomfort when participating in daily activities, such as walking or even wearing shoes. Proper footwear, cushioning, and moisture control are essential for preventing friction blisters. If a friction blister develops, it's important to cover it with a bandage or blister pad, rather than popping it, to minimize the risk of infection. Establishing a hygiene routine for your feet is advised to decrease the likelihood of friction blisters. Additionally, wearing moisture-wicking socks can help maintain a dry environment in your shoes. If you notice signs of a friction blister developing on the foot, it is suggested to discuss personalized care and treatment options with a podiatrist to alleviate discomfort and prevent future blisters.
Friction blisters of the feet are painful lesions caused by repetitive rubbing against the skin. These blisters typically occur on areas of the feet that experience frequent pressure or friction, such as the heels or toes. They appear as fluid-filled sacs beneath the top layer of skin and may cause discomfort when participating in daily activities, such as walking or even wearing shoes. Proper footwear, cushioning, and moisture control are essential for preventing friction blisters. If a friction blister develops, it's important to cover it with a bandage or blister pad, rather than popping it, to minimize the risk of infection. Establishing a hygiene routine for your feet is advised to decrease the likelihood of friction blisters. Additionally, wearing moisture-wicking socks can help maintain a dry environment in your shoes. If you notice signs of a friction blister developing on the foot, it is suggested to discuss personalized care and treatment options with a podiatrist to alleviate discomfort and prevent future blisters.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
Prevention & Treatment
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters are small pockets of fluid that occur on the top layers of the skin for several reasons. Friction, burns, and diseases are all known causes of blisters. Smaller blisters are known as vesicles, while larger blisters are referred to as bulla. The fluid inside the bubble can be blood, pus, or serum; which is a clear liquid that protects the skin. In most cases, blisters are not a major health issue, but they can be an indicator of a more serious condition.
Causes of blisters vary. Blisters are commonly caused by wearing poorly fitted shoes that rub against the foot. However, there are many other causes besides from friction; including burns, sunburn, insect bites, frostbite, poison ivy/oak, chemical exposure, impetigo, eczema, viral infections, and more.
Most blisters heal by themselves and do not require immediate medical care. If you have a blister, do not pop it since this may cause infection; it is advised to put a bandage over the blister to protect it. If the blister is large, causes pain, or if you have a fever, it is recommended that you see a doctor who can provide proper care. Blisters are easy to diagnose, and if considered prudent by the doctor, can easily be drained of fluid with a sterile needle as well.
To prevent blisters on the feet, wear shoes that fit properly and don’t cause rubbing. Socks can help prevent friction and it is recommended that you wear them if you are wearing shoes. Hand blisters can be avoided by wearing gloves during activities that cause friction against the hand. If you have a blister that pops, do not remove the dead skin, wash the area, apply antibiotic ointment, and cover with a bandage. It is okay in most cases to not seek immediate medical care for a blister if it was just caused by friction. However, if the blister causes pain or does not go away, it is suggested that you see a doctor for a diagnosis.
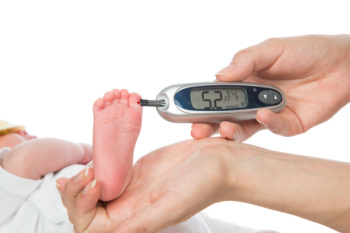 For people with diabetes, proper foot care is critical due to the risk of neuropathy and poor circulation, which can lead to severe complications. High blood sugar levels over time can damage nerves and reduce blood flow, causing numbness and decreased healing ability. This makes the feet more susceptible to injuries, infections, and ulcers, which can develop unnoticed and worsen quickly. To maintain foot health, individuals with diabetes should inspect their feet daily for cuts, blisters, redness, or swelling. Keeping feet clean and dry, moisturizing to prevent cracks, and trimming nails carefully are essential steps. Wearing properly fitted shoes and socks that reduce pressure and friction can prevent sores. Regular foot exercises and avoiding smoking may help to improve circulation. Failure to care for diabetic feet can lead to severe infections, gangrene, and even amputations. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist for regular check-ups and specialized treatment plans.
For people with diabetes, proper foot care is critical due to the risk of neuropathy and poor circulation, which can lead to severe complications. High blood sugar levels over time can damage nerves and reduce blood flow, causing numbness and decreased healing ability. This makes the feet more susceptible to injuries, infections, and ulcers, which can develop unnoticed and worsen quickly. To maintain foot health, individuals with diabetes should inspect their feet daily for cuts, blisters, redness, or swelling. Keeping feet clean and dry, moisturizing to prevent cracks, and trimming nails carefully are essential steps. Wearing properly fitted shoes and socks that reduce pressure and friction can prevent sores. Regular foot exercises and avoiding smoking may help to improve circulation. Failure to care for diabetic feet can lead to severe infections, gangrene, and even amputations. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist for regular check-ups and specialized treatment plans.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetes affects millions of people every year. Blood vessels located all over the body are damaged due to diabetes—even the blood vessels of the feet. Neuropathy, or nerve damage, can result from slower blood flow in the legs and feet. In diabetic patients, neuropathy is very important to monitor, as diabetics are at risk for developing ulcers.
Always washing and thoroughly drying the feet are pertinent parts of diabetic foot care. There should be a focus on cleaning between the toes. Even if no pain is felt, the entire foot should be examined for redness and sores. Neuropathy can often mask the pain of sores and ulcers and can cause these conditions to be overlooked. Use a mirror to examine the underside of your feet if needed. It is recommended that diabetics wear well-fitting socks.
Patients with diabetes should have their doctor monitor their blood levels because blood sugar levels play a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised. It is very important to keep your blood sugar levels in the normal range, which can be determined by your physician. There are medications that may be prescribed to help with any neuropathy experienced by the diabetic patient. It is also advisable to visit a podiatrist if one is experiencing any conditions involving the feet, such as ingrown toenails, which in more severe cases can cause infection.
Diabetic feet must be inspected daily. Diabetic foot care at home is possible if a patient is provided with instructions from their podiatrist. Patients can relieve dry heels with creams or ointments. Suspected wounds should warrant an immediate call to the podiatrist. Gangrene is a serious problem for diabetics and can lead to sepsis and amputation in its worst cases. Early treatment and daily inspection of diabetic feet are keys to staying healthy.

Foot fractures encompass a spectrum of injuries, each demanding specific attention and care. Among them, the Jones fracture affects the fifth metatarsal bone, typically requiring immobilization through casting or surgery to ensure proper healing. Metatarsal shaft fractures, occurring along the long bones of the foot, often necessitate rest, elevation, and the use of crutches to alleviate pressure. Proximal fifth metatarsal tuberosity avulsion fractures involve the pulling away of a small bone fragment due to sudden muscle contractions, often managed with immobilization and gradual return to weight-bearing activities. Additionally, big toe fractures, whether simple or complex, may require splinting, taping, or buddy taping to adjacent toes to promote stability. Relief techniques for foot fractures commonly involve rest and elevation to mitigate swelling and pain. Immobilization aids like casts, braces, or boots help stabilize the injured area, facilitating proper healing. If you have broken your foot, it is strongly suggested that you consult a podiatrist who can determine what type of fracture you have, and offer appropriate treatment methods.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Louisville Podiatry Office
149 Thierman Ln
Louisville,
KY 40207
Mon: 9:30 AM - 5:30 PM
Tues: 9:30 AM - 5:30 PM
Wed: 9:30 AM - 5:30 PM
Thur: 9:30 AM - 5:30 PM
Fri: 9:30 AM - 5:30 PM