
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.

Many people begin to develop balance problems as they age, putting them at a higher risk of falling. A few simple exercises can be done at home to improve health and mobility. (If you haven’t done any exercise in a while, it is always a good idea to check in with a health professional before embarking on any new program.) Just to be safe during these simple exercises, be sure to stand near a wall or chair, or keep a walking aid nearby before starting. It’s a good idea to start cautiously, building up the number of repetitions gradually to avoid injury. Heel-to-toe walk: Place the heel of your right foot directly in front of your left, looking straight ahead, and step down. Repeat 5 times. You may need to lightly touch the wall for stability. One-leg stand: Stand facing the wall, arms straight out in front, and lightly touch the wall in front of you. Lift one foot off the floor and hold for 5 -10 seconds. Repeat with the other foot. Do this 3 times. Sideways walking: Stand up straight with both feet together. Step out to the side with one foot, transfer your weight, and bring the other foot next to it. Repeat 10 steps. Then reverse direction. If you continue to experience balance problems, it may be a good idea to check in with a podiatrist for a complete biomechanical evaluation.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds, and every 19 minutes, an older person dies from falling. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
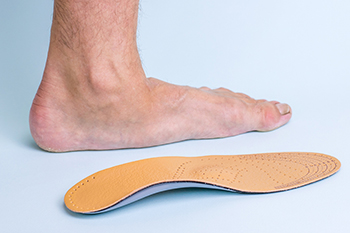
The feet, and the arch, bear the body’s weight, and provide support and shock absorption. The arch is composed of several different structures, with the ligaments providing the lion’s share of stability and support. Excessive forces placed on the feet due to obesity can change the foot’s structure, negatively affecting the ligaments of the arch, and even causing flat feet in many overweight people. Studies even suggest that the degree of an overweight person’s flat footedness is directly correlated to their level of obesity, with a higher Body Mass Index (BMI) correlated with a lower plantar arch height. People with flat feet might experience complications such as plantar fasciitis, muscle cramping, arthritis, Achilles Tendonitis, and other forms of foot discomfort or pain. A podiatrist can help anyone, regardless of weight, who is experiencing discomfort from flat feet with custom orthotic devices, supportive shoes, stretching exercises and stretches, physical therapy, pain management medication and more.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flatfoot is a foot condition in which the arch of the foot has either partially or totally dropped or has never developed. While it is common in babies and small children, it can become a problem for them in adulthood if the arch never forms. For adults, the development of flat feet can be brought upon by injury, as a result of pregnancy due to increased elasticity, or obesity. Those who have health concerns such as rheumatoid arthritis or diabetes may also be at greater risk for developing the condition.
If you suspect that you have flat feet, it is best to consult your podiatrist. Your foot doctor will examine the suspected foot and observe how it looks while you sit and stand. He or she may take an X-ray to determine how serious the condition is. Some common signs of flatfoot include toe drift, in which the toes and front part of the foot point outward, a short Achilles tendon, and a heel that tilts outwardly while the ankle tilts inward.
Once flatfoot has been diagnosed, your podiatrist may suggest one of several treatment options. Flat feet can be rigid, in which the feet appear to have no arch even when the person is not standing; or flexible, in which the person appears to have an arch while not standing, but once standing the arch disappears. Those with flexible flatfoot may be told to reduce any activities that cause pain and to avoid extended periods of walking or standing. Another suggestion may be weight loss, as excessive weight may be placing pressure on the arches
In few cases, if the condition is severe and all other methods have been exhausted surgery may be required. This is normally avoided, however, due to a lengthy recovery time and high cost.
 While pregnancy comes with innumerable joys, swollen feet are not one of them… Swollen feet are common among pregnant women and though not serious, can cause quite a bit of discomfort. Most foot swelling occurs in the latter part of a woman’s pregnancy, particularly in the second trimester, and it becomes noticeable around the third trimester. Beyond increased blood and fluids, the uterus becomes heavier as the baby grows and this can slow blood flow from the legs to the heart. Dietary issues, caffeine, insufficient water intake, hot weather, and being on one’s feet for long time periods can contribute to foot swelling during pregnancy. Again, all of this is normal though not fun, but it is important for moms-to-be to be aware of more serious conditions that may develop by monitoring sudden or dramatic increases in foot swelling. Regular consultation with a podiatrist can help pregnant women understand what to expect with their feet and legs during pregnancy.
While pregnancy comes with innumerable joys, swollen feet are not one of them… Swollen feet are common among pregnant women and though not serious, can cause quite a bit of discomfort. Most foot swelling occurs in the latter part of a woman’s pregnancy, particularly in the second trimester, and it becomes noticeable around the third trimester. Beyond increased blood and fluids, the uterus becomes heavier as the baby grows and this can slow blood flow from the legs to the heart. Dietary issues, caffeine, insufficient water intake, hot weather, and being on one’s feet for long time periods can contribute to foot swelling during pregnancy. Again, all of this is normal though not fun, but it is important for moms-to-be to be aware of more serious conditions that may develop by monitoring sudden or dramatic increases in foot swelling. Regular consultation with a podiatrist can help pregnant women understand what to expect with their feet and legs during pregnancy.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Many pregnant women complain about foot pain while they are expecting. Foot pain can primarily be caused by weight gain and hormonal changes taking place in the body. By understanding how pregnancy impacts the health of a woman's feet, a pregnant woman can take action to keep her feet as healthy and comfortable as possible.
Because a woman's weight changes during pregnancy, more pressure is brought to bear on both the legs and the feet. This weight shift can cause two major foot problems: over-pronation, also known as flat feet, as well as edema, which is swelling of the feet. Over-pronation occurs when the arch of the foot flattens, causing the foot to roll inwards when the individual is walking, and can aggravate the plantar fascia tissues located along the bottom of the feet. If these tissues become inflamed, a pregnant woman can experience pain in the heel of the foot as well as severe foot pain while walking or standing. Swelling of the feet, or edema, often occurs in the later stages of pregnancy. It is caused by slow circulation and water retention, and may turn the feet a light purple color.
To keep feet in good health and prevent over-pronation, pregnant women should avoid walking barefoot and be sure they are wearing shoes that offer good arch support. A device known as an orthotic can be added to regular footwear in order to provide additional support for the feet during pregnancy. Any expectant mother whose feet hurt should first check to see if the shoes she is wearing are old, worn out and not offering the proper support necessary for distributing the weight of her body during pregnancy.
To treat edema of the feet, a good start is to wear quality footwear which offers support and good circulation. Keep feet elevated whenever possible by using a foot stool while seated. Stay well hydrated by drinking plenty of water to prevent water retention in the feet. Any swelling that occurs in only one foot should be examined as soon as possible by a doctor.
Good foot health during pregnancy can help expectant mothers avoid foot pain that leads to other health problems. Massaging the feet and doing regular gentle exercise like walking aids foot health by contributing to good circulation. Supportive shoes are also a good investment that will support foot health during pregnancy.
Louisville Podiatry Office
149 Thierman Ln
Louisville,
KY 40207
Mon: 9:30 AM - 5:30 PM
Tues: 9:30 AM - 5:30 PM
Wed: 9:30 AM - 5:30 PM
Thur: 9:30 AM - 5:30 PM
Fri: 9:30 AM - 5:30 PM