
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
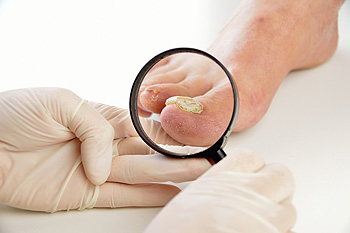 Toenail infections are a common problem that occurs when a fungus begins to grow under the nail. Upon infection, the toenail can turn yellow, become crumbly, thicken, and separate from the nail bed. Because the fungi that cause these infections thrive in warm and moist environments, there are a few key ways to prevent a fungal nail infection. These methods include ensuring that the feet are properly dried, keeping the toenails short, wearing clean socks, wearing footwear in public pools and showers, not sharing footwear with others, and using an antifungal spray in your shoes. If you still get an infection, there are a variety of treatment options that a podiatrist can provide. A podiatrist can prescribe antifungal medicines, remove the infected nail, or use an antifungal nail polish. If you believe that you have a fungal nail infection, visiting a podiatrist is recommended.
Toenail infections are a common problem that occurs when a fungus begins to grow under the nail. Upon infection, the toenail can turn yellow, become crumbly, thicken, and separate from the nail bed. Because the fungi that cause these infections thrive in warm and moist environments, there are a few key ways to prevent a fungal nail infection. These methods include ensuring that the feet are properly dried, keeping the toenails short, wearing clean socks, wearing footwear in public pools and showers, not sharing footwear with others, and using an antifungal spray in your shoes. If you still get an infection, there are a variety of treatment options that a podiatrist can provide. A podiatrist can prescribe antifungal medicines, remove the infected nail, or use an antifungal nail polish. If you believe that you have a fungal nail infection, visiting a podiatrist is recommended.
For more information about treatment, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
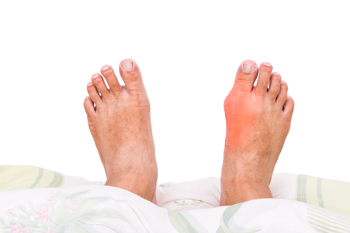 Bunions are a very common foot condition that cause a bony lump to form at the main joint of the big toe. This occurs when the joint is pulled out of alignment because the big toe is turned towards the rest of the toes. While bunions may not cause pain or symptoms at first, they can eventually push the other toes out of alignment making it difficult to wear shoes or walk. Bunions even have a tendency of causing skin irritation as the shoes rub against the affected area. Bunions can be caused due to inherited defects in the foot structure, wearing poorly fitted shoes, arthritis, conditions that damage the nerves in the feet, and of course injuries. If you are suffering from a painful bunion, consulting with a podiatrist for pain relief methods is highly suggested.
Bunions are a very common foot condition that cause a bony lump to form at the main joint of the big toe. This occurs when the joint is pulled out of alignment because the big toe is turned towards the rest of the toes. While bunions may not cause pain or symptoms at first, they can eventually push the other toes out of alignment making it difficult to wear shoes or walk. Bunions even have a tendency of causing skin irritation as the shoes rub against the affected area. Bunions can be caused due to inherited defects in the foot structure, wearing poorly fitted shoes, arthritis, conditions that damage the nerves in the feet, and of course injuries. If you are suffering from a painful bunion, consulting with a podiatrist for pain relief methods is highly suggested.
If you are suffering from bunions, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions are large bony bumps at the base of the big toe. Medically known as hallux valgus, a bunion is a misalignment of the metatarsophalangeal joint, or big toe joint. The misalignment will generally worsen with time if left untreated.
The exact cause of bunions is unknown, with genetics seen as a potential cause. High heels and poorly-fitted footwear, rheumatoid arthritis, and heredity all seem to be potential factors behind the exacerbation of bunions. Women have been found to be more likely to develop bunions in comparison to men.
Bunions do not always produce symptoms. The best way to tell is if the big toe is pushing up against the next toe and there is a large protrusion at the base of the big toe. You may or may not feel pain. Redness, swelling, and restricted movement of the big toe may be present as well.
Podiatrists use a variety of methods to diagnose bunions. If there are symptoms present, podiatrists will first consider that it is a bunion. If not, a physical examination will be conducted to check function of the big toe. Finally, an X-ray may be taken to view the extent of the bunion and confirm it is a bunion.
Typically, nonsurgical methods are used to treat bunions, unless the bunion has become too misaligned. Orthotics, icing and resting the foot, roomier and better fitted shoes, taping the foot, and pain medication are usually utilized first. If the bunion doesn’t go away or causes extreme pain, surgery may be required. Surgeons will either remove part of the swollen tissue or bone to straighten the toe out.
If you have a bunion, it is recommended to see a podiatrist. The longer it is left untreated, the worse it may get. Podiatrists can properly diagnose and treat a bunion before it gets worse.
 Research has indicated that frequent stretching and exercise may prevent falling episodes. This may be a result of the body becoming stronger as specific routines are performed, and falling may happen less often. Flexibility can be increased, and coordination and balance may also improve. Many injuries that can affect the feet can occur from falling, and this may cause difficulty in accomplishing daily activities. It is important to ensure the living environment is free of clutter, and it may help to install grab bars in the shower and toilet area. For added safety, many people choose to have a bath mat in the shower or tub area, as this can provide security. It is beneficial to have regular physical and eye examinations, as this may help to manage and update existing medication. If you would like additional information about how falling can impact the feet, please consult with a podiatrist.
Research has indicated that frequent stretching and exercise may prevent falling episodes. This may be a result of the body becoming stronger as specific routines are performed, and falling may happen less often. Flexibility can be increased, and coordination and balance may also improve. Many injuries that can affect the feet can occur from falling, and this may cause difficulty in accomplishing daily activities. It is important to ensure the living environment is free of clutter, and it may help to install grab bars in the shower and toilet area. For added safety, many people choose to have a bath mat in the shower or tub area, as this can provide security. It is beneficial to have regular physical and eye examinations, as this may help to manage and update existing medication. If you would like additional information about how falling can impact the feet, please consult with a podiatrist.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds, and every 19 minutes, an older person dies from falling. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
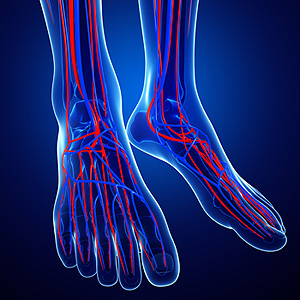 Raynaud’s disease is a disorder that causes temporarily reduced blood flow to the hands and feet. The reduction in blood flow is due to a contraction of the smooth muscles controlling the small arteries that supply blood to the hands and feet. This contraction is also known as a vasospasm. In people with Raynaud’s disease, vasospasms may be triggered by stress or cold temperatures. These can lead to the affected areas becoming numb, cool to the touch, and white or bluish in color. When blood flow returns to normal, the affected areas may throb, tingle, or turn red. If you have symptoms of Raynaud’s disease in your feet, a podiatrist can teach you how to manage this condition.
Raynaud’s disease is a disorder that causes temporarily reduced blood flow to the hands and feet. The reduction in blood flow is due to a contraction of the smooth muscles controlling the small arteries that supply blood to the hands and feet. This contraction is also known as a vasospasm. In people with Raynaud’s disease, vasospasms may be triggered by stress or cold temperatures. These can lead to the affected areas becoming numb, cool to the touch, and white or bluish in color. When blood flow returns to normal, the affected areas may throb, tingle, or turn red. If you have symptoms of Raynaud’s disease in your feet, a podiatrist can teach you how to manage this condition.
When dealing with systemic disease of the feet, it is extremely important to check the affected areas routinely so that any additional problems are caught quickly. If you have any concerns about your feet and ankles contact Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will assist you with all of your podiatric needs.
Systemic Diseases of the Feet
Systemic diseases affect the whole body, and symptoms usually are displayed in the feet. This condition can make a patient’s ability to walk unbearable. Systemic diseases include gout, diabetes mellitus, neurological disorders, and arthritis.
Gout – is caused by an excess of uric acid in the body. Common symptoms include pain, inflammation, and redness at the metatarsal/phalangeal joint of the base big toe. Gout can be treated by NSAIDs to relieve pain and inflammation, and other drugs that lower the acid levels in the body.
Diabetes mellitus – is an increase in the level of blood sugar that the body cannot counteract with its own insulin. Failure to produce enough insulin is a factor in Diabetes.
Diabetes of the Feet
Diabetic Neuropathy – may lead to damaged nerves and affect the feet through numbness and loss of sensation.
Peripheral Vascular Disease – can restrict the blood flow to the feet, and often times lead to amputation of the feet.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
There are several systemic diseases, or diseases that affect the whole body, that either display symptoms in the feet or affect the health of the feet. Common systemic diseases that affect the overall health of the feet, and the patient’s ability to walk comfortably, include gout, diabetes mellitus, neurological disorders, and arthritis, among others.
In gout, which is caused by an excessive buildup of uric acid in the body, the most common symptoms of pain, inflammation, and redness occur at the metatarsal/phalangeal joint at the base of the big toe. Any excess levels of uric acid crystallize and are deposited in tendons, joints, and surrounding bone and muscle tissue. Gout is commonly treated with NSAIDs to relieve pain and inflammation and other drugs to lower uric acid levels in the body. Gout most commonly affects those who are overweight, have low protein diets and lead a more sedentary lifestyle.
Diabetes mellitus is an increase in the level of blood sugar in which the body cannot counteract with naturally occurring insulin in the body. The three types of diabetes, Type I, Type II and Gestational Diabetes, are all signs the body is either not producing enough insulin or is not efficiently using the insulin that is produced. Gestational diabetes only affects women who are pregnant and have never, prior to pregnancy, exhibited symptoms of the disease.
There are two main issues that affect the feet that are commonly caused by diabetes. They include diabetic neuropathy and peripheral vascular disease. Diabetic neuropathy can lead to damaged nerves and affect the feet through numbness and loss of sensation. Peripheral vascular disease restricts the flow of blood to the foot and can, in extreme cases, lead to the necessity of amputating the foot. Peripheral issues that are caused by diabetes and can affect the foot include athlete’s foot, nail infections, corns, blisters, bunions, severe dry skin, plantar warts and ingrown toenails. These can all be attributed to the decrease of blood flow to the foot.
Neurological disorders and rheumatoid arthritis can also have severe impact on the health of the feet. Neurological disorders can affect the nerves in the main structure of the foot and cause loss of sensation and possible decreased muscle response. Rheumatoid arthritis can affect the bones and joint structures of the foot, making it impossible to walk normally without serious pain.
All systemic diseases that affect the foot can effectively be treated to minimize joint and muscle damage if they are diagnosed early and treated with medication and lifestyle therapy. Diabetes patients must monitor their blood sugar levels and work with their physician to keep their levels as close to normal as possible. Rheumatoid arthritis patients should work with their physician to ensure the proper medications are being taken to reduce the amount of damage to the joints of the body.
Louisville Podiatry Office
149 Thierman Ln
Louisville,
KY 40207
Mon: 9:30 AM - 5:30 PM
Tues: 9:30 AM - 5:30 PM
Wed: 9:30 AM - 5:30 PM
Thur: 9:30 AM - 5:30 PM
Fri: 9:30 AM - 5:30 PM