
 Peripheral artery disease, or PAD, is a condition where the arteries that supply blood to the legs and feet become narrowed or blocked due to plaque buildup. This decreases blood flow to the lower extremities. Symptoms of PAD can vary but often include leg pain or cramping while walking or climbing stairs, which typically eases with rest. Some people may also experience numbness, weakness, or a cold sensation in their lower legs or feet. Changes in the color of the skin or slower growth of the nails may also occur. In more severe cases, PAD can lead to wounds or ulcers on the feet or legs that heal poorly or not at all. Getting diagnosed early is important because PAD can be a sign of more widespread arterial disease, which could increase the risk of heart attack or stroke. Early treatment can help manage symptoms, improve mobility, and reduce the risk of more serious complications. It is suggested that you consult a podiatrist, or foot doctor, for help if you are experiencing any symptoms that sound like PAD.
Peripheral artery disease, or PAD, is a condition where the arteries that supply blood to the legs and feet become narrowed or blocked due to plaque buildup. This decreases blood flow to the lower extremities. Symptoms of PAD can vary but often include leg pain or cramping while walking or climbing stairs, which typically eases with rest. Some people may also experience numbness, weakness, or a cold sensation in their lower legs or feet. Changes in the color of the skin or slower growth of the nails may also occur. In more severe cases, PAD can lead to wounds or ulcers on the feet or legs that heal poorly or not at all. Getting diagnosed early is important because PAD can be a sign of more widespread arterial disease, which could increase the risk of heart attack or stroke. Early treatment can help manage symptoms, improve mobility, and reduce the risk of more serious complications. It is suggested that you consult a podiatrist, or foot doctor, for help if you are experiencing any symptoms that sound like PAD.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.

Ensuring proper shoe fit goes a long way in preventing heel pain, where both support and comfort play pivotal roles. Wearing ill-fitting shoes, particularly high heels, and narrow styles, exacerbate heel discomfort by placing excessive pressure on the heel and altering natural foot mechanics. During the pandemic, the widespread adoption of unsupportive footwear like slippers and flip-flops further contributed to foot problems, as they lacked adequate arch support and cushioning. As individuals age, foot structures change, making them more susceptible to heel pain. Therefore, it is imperative to prioritize footwear that offers ample support and cushioning to alleviate strain on the heels and promote proper alignment. Opting for shoes with a wide-toe box, cushioned insoles, and low to moderate heels can help distribute weight evenly and reduce heel pain. If you suffer from persistent heel pain, it is strongly suggested that you schedule an appointment with a podiatrist who can diagnose the cause and offer guidance on the best shoes to wear for your particular needs and circumstances.
Many people suffer from bouts of heel pain. For more information, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.
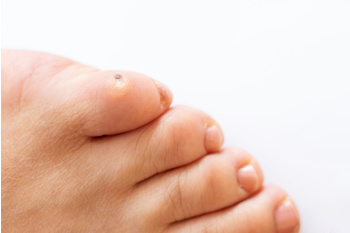
Corns on the feet, medically termed keratotic lesions, are areas of thickened skin caused by repeated friction or pressure. They commonly occur on weight-bearing areas like the toes and soles of the feet. Symptoms can include localized pain or tenderness, a hardened or raised bump, and sometimes inflammation or redness. Older individuals are more prone to developing corns due to factors like reduced skin elasticity and altered foot mechanics. There are three main types of corns. Hard corns are small, dense, and are usually found on bony areas. Soft corns are moist and typically form between toes where the skin is moist. Seed corns are tiny and appear on non-weight-bearing areas. Diagnosis is typically made based on clinical examination. Management involves relieving pressure on the affected area, wearing properly fitting footwear, using protective pads or cushions, and sometimes, having the corn removed. If you have persistent or painful corns, it is suggested that you schedule an appointment with a podiatrist for treatment.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact Dr. Steven Shlonsky of Louisville, Kentucky. Dr. Shlonsky will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Corns are thickened areas on the skin’s surface, to the point of being irritating and sometimes painful. Commonly found on the feet, corns are circular or cone-shaped. They develop where there are areas of pressure or friction, such as on the little toe when it rubs up against shoes, or on the ball of your foot.
Corns are often confused with a callus, but there is a difference between them. Corns can be raised bumps that are painful to the touch. They consist of a rough, thick area of skin that may be dry or waxy. Corns tend to be surrounded by skin that is inflamed, and are usually much smaller than calluses.
Removing the dead skin that has built up is the key in treating corns. Salicylic acid medication is most common in accomplishing this. The acid works by dissolving keratin, which is the protein that makes up the majority of corns. You can purchase salicylic acid over-the-counter in products such as wart removers. It comes in a variety of forms such as medicated pads, drops, or creams. However, people who are diabetic should not use salicylic acid, but should instead consult their doctor immediately.
According to the product directions, applying the medication directly onto the corn will treat it. The top layer of the corn will begin to turn white after use. When that occurs, the layers of skin can then be peeled away, making the corn smaller. Shaving off corns with razors or other pedicure equipment is never a good idea. This can lead to infection. If your corn gets infected, and is not treated immediately, a visit to the doctor will be necessary.
Another way to treat corns and help prevent their return is by using orthotic inserts, fitted by a podiatrist. Inserts fit right into your shoes and adjusts the way your foot fits into your shoes. This fixes the way you walk. This will lower your chances of getting corns, and eliminate current corns by reducing rubbing from friction.
Surgery is rarely used to treat corns, but does occur on occasion. Surgery actually deals with the underlying issue that causes corns. During surgery, the bone is shaved and any abnormalities are corrected, thus reducing the amount of friction that occurs during walking.
To prevent corns, the first step is reducing friction. Always wear shoes that fit well and don’t rub your feet. Pads can be purchased if you notice rubbing developing. These pads can be purchased over-the-counter, and can be simply placed on the irritated area. Wearing cushioned insoles in your shoes can always reduce the friction, and making sure to wear well-fitting shoes. This will ensure that your foot is not being squeezed awkwardly, and prevent corns from forming in the first place.

Exercise is an important way to reduce the risk of falling, particularly by focusing on activities that improve muscle strength, balance, posture, and stamina. Muscles naturally weaken and balance deteriorates without consistent exercise. By incorporating simple exercises into your daily routine, you can significantly increase stability and help prevent falls. Be sure to have a chair or counter nearby for safety reasons. Try standing on tiptoes, gradually transitioning to heel lifts and toe raises to improve ankle strength and balance. Side leg raises, performed by lifting one leg to the side while keeping toes forward, are excellent for strengthening hip abductors and improving lateral stability. Additionally, practicing walking in a straight line, progressing by placing one foot directly in front of the other to walking heel to toe along a counter. This can enhance overall balance and coordination. Sometimes, underlying foot or ankle issues contribute to instability. If balance issues have become a problem, it is suggested that you make an appointment with a podiatrist to address them.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds, and every 19 minutes, an older person dies from falling. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
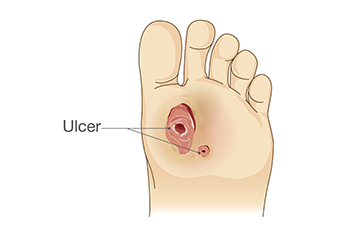
Patients with diabetes face an increased risk of developing foot ulcers, or slow-healing sores, as the result of nerve damage and compromised blood circulation. Around 20 percent of people with diabetes experience a foot ulcer at some point in their lives. About half of these ulcers may become infected, which can bring serious complications, including gangrene and possibly amputation. Factors such as loss of sensation in the feet, poor circulation, and foot deformities heighten the likelihood of developing diabetic foot ulcers. Other risk factors include vision impairment, difficulty with foot care, or a prior history of ulcers. Regular foot examinations by a podiatrist are important for early detection and intervention. If you're experiencing foot problems related to diabetes, it is suggested that you make regular appointments with a podiatrist who is trained to deal with these issues.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Steven Shlonsky from Louisville, Kentucky. Dr. Shlonsky can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Louisville, KY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Louisville Podiatry Office
149 Thierman Ln
Louisville,
KY 40207
Mon: 9:30 AM - 5:30 PM
Tues: 9:30 AM - 5:30 PM
Wed: 9:30 AM - 5:30 PM
Thur: 9:30 AM - 5:30 PM
Fri: 9:30 AM - 5:30 PM